Anaheim, Calif.—The leading cause of death in breast cancer patients today is heart disease. Women in their 40s and 50s are experiencing heart failure and other cardiotoxicities after treatment with radiation, anthracyclines and HER2 receptor antagonists, noted Sandra Cuellar, PharmD, BCOP, at the 13th Annual Conference of the Hematology/Oncology Pharmacy Association.
“It’s no longer that they are diagnosed with breast cancer and they are dying of breast cancer. They are dying of heart disease,” said Dr. Cuellar, a clinical assistant professor and clinical oncology pharmacist at the University of Illinois Hospital and Health Sciences System, in Chicago.
However, if women receive cardioprevention within two months after cancer treatment, the cardiomyopathies could be mitigated and even reversed. In addition, the definition of high-dose anthracycline has changed, which should help mitigate some of the risks.
“For decades, we were taught it was a lifetime cumulative dose of 400 to 500 mg/m2. Now, ASCO [American Society of Clinical Oncology] guidelines state [the] high dose is 250 mg/m2 or more, meaning the threshold is almost half of what we had thought,” Dr. Cuellar explained. “We have to retrain ourselves to this new threshold.”
The new guidelines “are game changers,” added Dr. Cuellar, who joked that the data gave her tachycardia. “We know we are going to cause cardiotoxicity, but there may be something we can do about it.”
The average five-year survival rate for individuals with breast cancer is 89%; the 10-year rate is 83%; and the 15-year rate is 78%, according to ASCO data. If the cancer is located only in the breast, the five-year relative survival rate for breast cancer is 99%.
“One of the bright sides about the statistics is that we have more breast cancer survivors,” she said. “Unfortunately, we have a dark side to this statistic in that there are more women who are diagnosed with heart failure and cardiomyopathy.”
Dr. Cuellar discussed some of the drug cardiotoxicities. A retrospective study of almost 12,000 women found that the risk for HF after anthracyclines was 1.4 times that of women who did not receive anthracyclines (J Natl Cancer Inst 2012;104[17]:1293). If they took trastuzumab (Herceptin, Genentech) alone, it was fourfold higher; if they required a combination of anthracyclines and trastuzumab, they had a sevenfold increase in cardiomyopathies, she said.
The timing of the cardiomyopathies is important to consider, she noted. Their incidence is fairly low one year after treatment: With an anthracycline, 1% of treated women will have a cardiomyopathy; with trastuzumab, almost 4%; and for combination therapy, 6.2%. But five years after treatment, the numbers increase dramatically. For anthracycline alone, 4% of women will have a cardiac event, such as HF. For trastuzumab, 12% of women will have cardiotoxicity. For combination treatment, it’s 20%. “Twenty percent of women who had combination anthracycline plus trastuzumab, at year 5 are having cardiomyopathy,” Dr. Cuellar said. “And we are seeing this time and time again.”
Only 25% of breast cancer patients have a cardiac comorbidity at diagnosis (Breast Cancer Res 2011;1-9). “That means that 75% developed a cardiac comorbidity after their breast cancer diagnosis, and subsequently die of that cardiac comorbidity,” she said.
Curative Here, Poison There
“A hallmark lesson we teach pharmacy students is that a treatment in one part of the body can be a poison elsewhere,” said C. Michael White, PharmD, FCP, FCCP, a professor and the head of the Department of Pharmacy Practice at the University of Connecticut School of Pharmacy, in Storrs, and a specialist in cardiology. “Treating breast cancer effectively puts the heart at risk. We have to find ways to mitigate that risk without watering down the benefits for the cancer so we can maximize the risk–benefit ratio.”
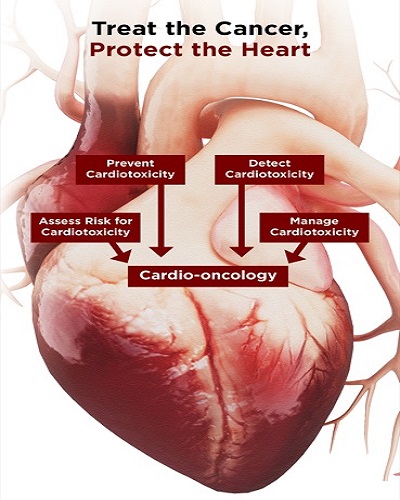
The cancer–cardiotoxicity statistics are changing the relationship between oncologist and cardiologist, according to Dr. Cuellar. “Cardio-oncology is emerging as a subspecialty,” she said, and patients should be seeing a cardiologist before, during and after treatment.
The same lifestyle risks—hypertension, diabetes, dyslipidemia, obesity, smoking—that increase the risks for cardiovascular disease for everyone also occur in patients with breast cancer, and compound their risks. One component of the ASCO Breast Cancer Survivorship Guidelines says that breast cancer survivors should be educated about potential risk factors and healthy lifestyle modifications, and be monitored for cardiovascular disease throughout their lives after treatment (CA Cancer J Clin 2016;66[1]:43-73).
The cardiovascular risk is so high among many different types of cancer, not just breast cancer, that ASCO recently issued a guideline for preventing and monitoring cardiac dysfunction in adult cancer survivors (J Clin Oncol 2017;35[8]:893-911).
ASCO recommends preventive strategies to reduce the risks. “The goal should be to treat cancer while protecting the heart,” Dr. Cuellar said.
Prophylaxis a Mixed Bag
The data are limited on using pharmacologic agents, such as beta blockers and ACE inhibitors, during treatment. The MANTICORE-101 (Multidisciplinary Approach to Novel Therapies in Cardiology Oncology Research) trial found that giving perindopril or bisoprolol during treatment with HER2 receptor antagonists protected against a decline in left ventricular ejection fraction, but did not prevent left ventricular remodeling (J Clin Oncol 2016;34:1-7).
But providing such medications within a few months of treatment, while the heart disease is subclinical, could greatly mitigate or reverse the disease, according to Dr. Cuellar. In another trial, 64% of patients who were given heart drugs within two months of anthracyclines responded to treatment. If the drugs were delayed between two and four months, the response rate was 28%. If they were delayed between four and six months, the response rate was 7%, and with treatment after six months, there was no response (J Am Coll Cardiol 2010;55:21-20).
Therefore, the ASCO guidelines recommend follow-up of breast cancer patients before, during and after treatment. Patients should receive a risk assessment with recommendations for lifestyle changes. They should receive diagnostic imaging and cardiac biomarker measurements and be treated promptly if there are signals of subclinical heart disease. Do not wait for symptoms, Dr. Cuellar said.
Dr. White agreed that early intervention can make all the difference. “Treating [other] patients with both beta blockers and angiotensin II inhibiting drugs within the first day of a myocardial infarction pays major dividends in protecting ejection fraction, and it seems realistic that it could also benefit patients where the insult is due to breast cancer drugs,” he said. “Of course, further work needs to be done to know how valuable this type of prophylaxis could be, but it is heartening that researchers are going down this path.”
ECHO imaging with global longitudinal straining and cardiac biomarkers, such as troponin, have emerged as the most useful methods for detecting subclinical abnormalities before the patients suffer a decrease in left ventricular function, according to Dr. Cuellar.
“We have always been taught that heart failure from anthracycline therapy was irreversible, but these data suggest that maybe it is reversible,” she said. “Because we were never aggressive about detecting it, by the time patients were symptomatic, it was already irreversible. We want to intervene when that subclinical dysfunction occurs.”
—Marie Rosenthal